The short answer is yes, but only in limited cases. The Canadian Dental Care Plan (CDCP) does offer some orthodontic coverage; however, it is not available for everyone, and it does not cover the full cost of braces in most situations. If you are a Canadian resident wondering whether you or your child can get braces covered under the CDCP, you are in the right place. At North York Smile Avenue Dentistry, we work with patients every day who have questions about what the CDCP covers and how to make the most of their benefits. In this guide, we break down exactly who qualifies, what is covered, how much you can expect to pay, and what your options are if you do not qualify. Keep reading so you do not miss any important details that could save you thousands of dollars.
Understanding the Canadian Dental Care Plan (CDCP)
The Canadian Dental Care Plan is a government program launched in 2024 to help Canadians who do not have private dental insurance pay for dental care. It is designed for low to middle-income residents who would otherwise struggle to afford dental treatments. The plan is managed through Sun Life Financial and covers a range of dental services depending on your income level and the type of treatment you need. To qualify, you must be a Canadian resident, have a family income below a certain threshold, and have no access to private dental insurance. Understanding how the plan works is the first step to knowing whether braces or other orthodontic treatments can be covered for you or your child.
Does the CDCP Cover Braces?
The CDCP does include some orthodontic coverage, but it is very limited and comes with strict conditions. Braces are not covered as a cosmetic treatment, which means if you want straighter teeth for appearance reasons only, the plan will not help you. However, if braces are considered medically necessary, such as in cases where a child has a severe bite problem or a jaw issue that affects their ability to chew or speak, the plan may cover part of the cost.
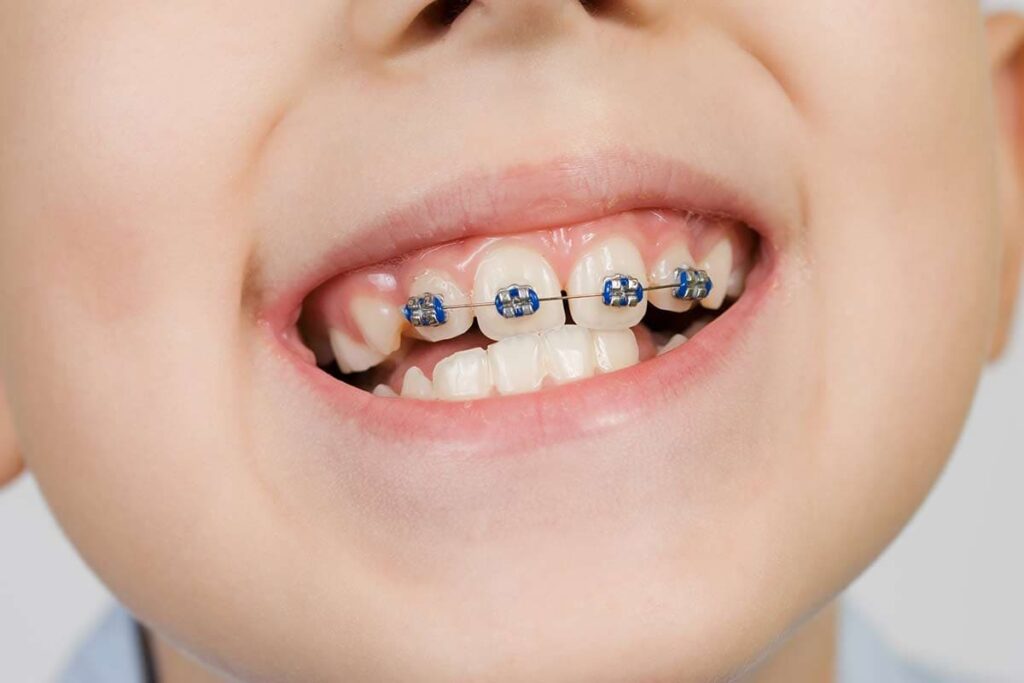
Based on what we see at Smile Avenue Dentistry, most approved orthodontic cases under the CDCP involve children with significant functional issues rather than mild alignment concerns. Our dental team reviews each patient’s situation carefully to determine whether their case meets the medical necessity requirements set by the plan. If you are unsure whether you or your child qualifies, the best step is to book a consultation so we can assess your case and guide you through the process honestly and clearly.
Read More: CDCP for Children: What Parents Need to Know
What Types of Orthodontic Treatments Might Be Eligible?
Based on the current CDCP guidelines and what we see in our practice, coverage is limited to treatments that are considered medically necessary rather than cosmetic. Here are the types of orthodontic treatments that may be eligible under the plan:
- Traditional Metal Braces:
Metal braces are the most commonly approved orthodontic treatment under the CDCP. They are typically considered when a patient has a severe malocclusion or bite issue that affects their daily function, like chewing or speaking properly.
- Interceptive Orthodontics:
This is an early treatment approach used for younger children whose jaw and teeth are still developing. If a child shows signs of serious bite problems at an early age, interceptive orthodontic treatment may qualify for partial coverage under the plan.
- Removable Appliances:
In some cases, removable orthodontic appliances like expanders or retainers that are part of a medically necessary treatment plan may be covered. These are usually recommended alongside other orthodontic work rather than as a standalone treatment.
- What Is Unlikely to Be Covered:
Clear aligners like Invisalign are generally not covered under the CDCP because they are considered a cosmetic or elective option in most cases. Cosmetic tooth straightening without a functional diagnosis is also unlikely to qualify.
How Much Do Braces Cost With CDCP?
One of the most common questions we hear from patients is how much they will actually pay out of pocket for braces after their CDCP benefits are applied. The plan uses an income-based co-payment system, so the amount you pay depends on your household income. Families earning under $70,000 can have up to 80 percent of eligible costs covered, while those earning between $70,000 and $79,999 receive around 60 percent coverage. Coverage drops to about 40 percent for incomes between $80,000 and $89,999 and down to 20 percent for incomes between $90,000 and $99,999. Keep in mind that these percentages only apply to the eligible portion of the treatment cost based on the CDCP fee guide, and if your provider charges above that rate, you will be responsible for the difference. Our team at Smile Avenue Dentistry always walks patients through the full-cost breakdown before starting any treatment, so there are never any surprises.
Read More: How Much Do Braces Cost in Canada?
Who Qualifies for Orthodontic Coverage Under the CDCP?
Not everyone who needs braces will qualify for orthodontic coverage under the CDCP, so it is important to understand the criteria before you apply. To be eligible, you generally need to meet all of the following conditions:
- You must be an active CDCP member with a family income below $100,000 and no access to private dental insurance
- The treatment must be medically necessary and supported by clinical documentation from your dental provider
- Your case must meet a minimum severity level, as mild cosmetic alignment issues are not covered
- Prior authorization from Sun Life Financial must be approved before treatment begins
Read More: CDCP Eligibility: Who Can Access Canadian Dental Care in 2026?
How CDCP Orthodontic Coverage Compares to Private Dental Insurance
If you are trying to decide whether the CDCP is enough for your orthodontic needs or whether private dental insurance offers better value, it helps to see them side by side. Here is a clear comparison:
| Feature | CDCP | Private Dental Insurance |
|---|---|---|
| Who it is for | Low to middle-income Canadians with no private insurance | Anyone who purchases a plan or receives coverage through an employer |
| Orthodontic coverage | Limited to medically necessary cases only | Often covers a portion of braces for both children and adults |
| Coverage amount | 20% to 80%, depending on family income | Typically, around 50% up to a lifetime maximum |
| Cosmetic treatment | Not covered | Sometimes covered, depending on the plan |
| Prior authorization | Required for all orthodontic treatments | Required by most plans |
| Clear aligners (Invisalign) | Generally not covered | Covered by some plans |
| Annual or lifetime maximum | Set by CDCP fee guide | Varies by plan, usually $1,500–$3,000 lifetime |
| Cost to you | Free to enroll | Monthly premiums apply |
What Orthodontic Services Are NOT Covered?
Many patients are surprised to find out how limited the CDCP orthodontic coverage actually is. Knowing what is not covered before you start treatment can save you from unexpected costs. Based on the current plan guidelines, the following services are generally not covered:
- Braces or aligners for cosmetic reasons, with no functional diagnosis
- Clear aligners like Invisalign are considered elective in most cases
- Mild crowding or spacing issues that do not affect chewing or speaking
- Retainers that are not part of an approved treatment plan
- Any treatment that begins before prior authorization is granted by Sun Life Financial
What Is Covered by the CDCP?
On the other side of the coin, the CDCP does offer real help for patients who meet the eligibility requirements. Here is what is generally covered:
- Diagnostic records, like X-rays and assessments needed to support your claim
- Traditional metal braces when treatment is medically necessary and pre-approved
- Interceptive treatment for children with significant developmental issues
- Removable appliances that are part of an approved treatment plan
- Follow-up visits are directly related to an approved orthodontic treatment
Read More: How to Find a CDCP Dentist Near You
Alternatives If Braces Aren’t Covered
If your orthodontic treatment is not covered under the CDCP, there are still several ways to make braces more affordable. At Smile Avenue Dentistry in North York, we always make sure our patients leave with a clear plan, regardless of their coverage situation. Here are some options worth exploring:
- Ask your dental office about flexible in-house payment plans that let you spread the cost over time
- Check local community health centers or public health programs that offer reduced-cost dental care
- Consider accredited dental schools where orthodontic treatment is offered at a lower cost under professional supervision
- Reassess your CDCP eligibility every year, as your income or insurance situation may change, and you could qualify in the future
Not sure if your braces qualify under CDCP?
Book a consultation with our dental team to check your eligibility and explore covered orthodontic options.
FAQ
Does CDCP orthodontics cover Invisalign cost?
No. Invisalign is considered an elective and cosmetic treatment, so it is not covered under the CDCP. Only medically necessary orthodontic treatments like traditional metal braces may qualify.
How Long Does It Take to Get Pre-Approval?
The pre-approval process through Sun Life Financial typically takes a few weeks. Your dental provider needs to submit a full treatment plan along with clinical records before any treatment can begin, so it is important to start this process early.
Are braces free under CDCP?
Not completely. The CDCP covers a percentage of the eligible treatment cost depending on your family income. You will still have an out-of-pocket portion to pay, and any costs above the CDCP fee guide are also your responsibility.
Does CDCP cover orthodontics for adults?
Adults can apply for orthodontic coverage, but approval is much less common. The treatment must be medically necessary, and the bar for proving that is generally higher for adults than for children.
Do children get better orthodontic coverage?
Yes. Children and teenagers with significant functional or developmental bite issues are more likely to be approved for orthodontic coverage under the CDCP compared to adults.